Pain is rarely easy. It drifts throughout cells, nervous system, cognition, and context. Physiotherapists rest at the crossroads of all of it, asked to ease pain while recovering function under time pressure and facility restraints. The most effective pain monitoring courses do not hand out a bag of techniques. They hone medical reasoning, strengthen expertise of systems, and refine hands-on skills and modality options so you can meet the certain person in front of you. This overview walks through how solid training programs are constructed, where manual treatment and modalities really fit, and exactly how to choose a program path that matches your caseload, setting, and scope.
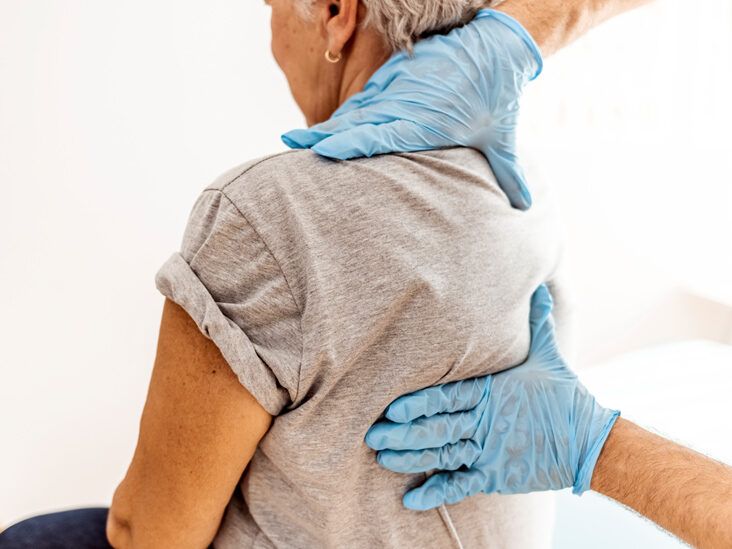
Where discomfort training fulfills practice
A new grad frequently arrives at their very first bone and joint facility with confident palpation abilities and a collection of workouts. Within months the outliers show up. A 42‑year‑old roofer with consistent shoulder pain regardless of an ideal cuff protocol. A marathoner whose hamstring pain flares long after the tear has actually recovered. A nurse that can not shake low pain in the back after a minor lifting event, now made complex by fatigue and bad rest. These cases are not failings of the therapist or the individual. They are signals that pain is not only a cells problem. Discomfort monitoring courses for physio therapists fill the gap in between conventional rehab and the useful facts of nociplastic pain, main sensitization, and changing psychosocial loads.
When people ask which pain administration training course to take, they generally imply 2 points. They desire better hands, and they desire smarter decisions. The answer is an educational program that appreciates both.
Manual treatment's role today
Manual treatment continues to be a staple, however a lot of seasoned clinicians rectify their expectations with time. It is less about fixing a sore and even more about modulating the system. Joint strategies can bring back tolerance to motion. Soft tissue techniques can minimize safety tone. Nerve sliding can desensitize irritated user interfaces. None of it treatments neck and back pain in one session, and none of it is worthless. The technique is adjusting dose and intent, after that coupling hands-on input with activity and education.
A solid manual‑focused pain monitoring program reveals you:
- How to use manual input as a short‑term home window to allow rated direct exposure, not as a standalone cure. How to pick methods matched to sign habits and mechanism: high impatience gets gentle, non‑provocative application; low impatience endures much more details packing and mobilization. How to interact about hand-operated therapy without enhancing fragility: clarify comfort and activity gain, not "putting points back in position."
In technique, I commonly run a simple experiment during the initial session. Apply a low‑dose method, then quickly retest the person's significant job, like sit‑to‑stand, reach, or step‑down. If discomfort decreases or confidence increases, we bank the gain with two minutes of movement in that brand-new home window. If nothing modifications, penalty, we carry on. Manual inputs are levers, not magic.
Modalities without the myth
Electrotherapy, laser, shockwave, ultrasound, warmth, and chilly each have advocates and doubters. In pain management training, the sober center path is best. Ask 3 inquiries. Does this method have at least moderate proof for this condition or device? Will it open a home window to motion or feature? What chance cost does it introduce in time or money?
Take TENS. Analgesic effects are genuine for some individuals, specifically for short‑term relief in severe flares, painful procedures, or when medicine is restricted. It overcomes segmental inhibition and coming down modulation. However the result discolors when it stops, and the magnitude is variable. Shockwave has a duty in stubborn tendinopathies if loading has actually plateaued and the patient understands that it is an accessory, not the main event. Healing ultrasound stays reduced worth for a lot of MSK discomfort, with exemptions in targeted bone recovery protocols where tool and criteria issue. Warm is undervalued for high‑guard states and sleep preparation. Ice aids with severe irritation and swelling, however it can not outrun tons mismanagement.
Courses that deal with methods as devices with trade‑offs, not identity pens, prepare you for real clinics where time is short and co‑payments are real.
Understanding mechanisms without losing the patient
The language of discomfort science has actually matured. Nociception differs from discomfort. Central sensitization can magnify signals even when tissues are healing. Context shifts discomfort obtain up or down. Good programs translate these principles right into professional moves.
One technique I educate is the triad: system hypothesis, irritability, and dominant limiter. Mechanism asks whether nociceptive vehicle drivers, neuropathic features, or nociplastic patterns are primary. Impatience establishes dose. The dominant limiter identifies what is choking operate now: anxiety, rest, deconditioning, inflammatory tons, or a details mechanical limitation. As soon as those three are clear, hand-operated choices and techniques form instead of determining the plan.
A short example. A 36‑year‑old with posterior thigh pain after a sprint. MRI reveals a grade II hamstring pressure that is currently eight weeks old. She reports twinges when flexing to connect shoes, protected stride, and bad sleep. Checking discloses reasonable strength yet high level of sensitivity to stretch. System: primarily nociceptive with a sensitized interface. Impatience: modest. Dominant limiter: motion concern plus level of sensitivity to neurodynamics. Strategy: begin with gentle hand-operated strategies around the posterior chain to lower guarding, add slider‑style nerve mobilization, supply clear education and learning concerning risk-free discomfort, and start graded filling in mid‑range. Consider brief bursts of 10s throughout the first week to alleviate excruciating jobs. Reflect on regular and taper the techniques as self-confidence rises.
What a well balanced pain monitoring curriculum covers
Good discomfort administration training courses for physiotherapists develop split capability instead of a solitary specific niche. Several aspects are non‑negotiable.
- Pain devices and scientific thinking. You must complete able to protect a strategy in ordinary language to a person and in accurate terms to a colleague. Manual therapy abilities with application. Not simply methods, but when and exactly how to quit, switch over, or pair with movement. Modality rationales and parameters. Practical, condition‑specific guidance with clear caveats. Communication and expectations. Scripts and allegories that de‑threaten without lessening the patient's experience. Graded exposure and tons layout. Running progressions, return‑to‑work ladders, lifting build‑ups, and flare‑up protocols. Sleep, tension, and task preparation. Simple levers with outsized impact. Outcome procedures that direct adjustment. Usage quick devices like discomfort interference, sleep top quality ratings, and task‑specific scores, not simply variety of motion.
Programs that weave these themes throughout instance conversations and live laboratories leave you prepared to handle a messy caseload on Monday morning.
Certificates, brief training courses, and the alphabet soup
Many physio therapists ask about a pain monitoring certification or discomfort monitoring accreditation that signifies depth. The worth depends on your area and employer expectations. Some health systems acknowledge organized certificate training course hurting monitoring pathways that consist of a capstone and exam. Others care more about portfolio and results. Short courses hurting administration are often the most effective entry point if you want concentrated skills without a multi‑month commitment. Weekend intensives on hand-operated therapy application, or two‑day workshops on rated electric motor images and desensitization, can move your practice quickly when complied with by intentional practice.
If your clinic offers intense care, consider emergency situation pain administration components. They cover triage of warnings, fast analgesic approaches that play well with clinical procedures, and secure early mobilization for rib cracks, acute neck discomfort after small accidents, or low neck and back pain in the ED. The goal is not to change medicine however to supply movement‑based analgesia and minimize time to discharge.
Some vocational and first‑aid frameworks consist of the code PUAEME008. It involves elements of offering pain administration in emergency setups within specified range. While designed for emergency situation feedback contexts, the frame of mind carries over: clear evaluation, early analgesia techniques, secure positioning, and measured rise. If your function includes sideline coverage or neighborhood event assistance, reviewing PUAEME008 supply pain monitoring material can hone your decision‑making and interprofessional interaction. That said, physio therapists commonly depend on non‑pharmacological approaches unless local plan and credentialing give otherwise.
Tailoring for certain populations
The best training courses recognize that different settings alter the playbook.
Sports and high‑performance. Manual therapy and methods typically serve to regulate signs between training lots. Professional athletes worth time‑efficient modifications. A five‑minute peripheral nerve technique followed by a run mechanics drill can be more influential than a lengthy lecture on discomfort physiology. Shockwave shows up at the edges for calcific tendinopathy or chronic plantar fasciopathy when loading and education and learning have plateaued.
Spine hefty outpatient facilities. Education practices matter greater than any type of device. Show discomfort variability as typical, use traffic‑light systems to handle flare‑ups, and prescribe activity treats. Hands-on therapy dosages are tiny and frequent, after that tapered, while the exercise program rises from tolerance to capacity. Warm and TENS can assist oversleep the initial two weeks.

Pelvic wellness. Discomfort level of sensitivity, trauma background, and privacy call for splendid communication. Manual labor is mild and consent‑forward. Psychophysiological feedback and breathing patterns are frequently the first modalities, with warmth and desensitization workouts as follow‑ups. Training courses in this domain name need to courses for nurses in pain management consist of interdisciplinary recommendation pathways.
Neuropathic pain discussions. When the system leans neuropathic, such as post‑surgical nerve pain or radiculopathy without progressive shortage, hand-operated treatment targets interfaces and securing while education and learning focuses on nerve wellness and blood circulation. Rated exposure blends isometrics, sliders, and targeted aerobic job. 10s or scrambler treatment may contribute depending on schedule and individual preference.
Persistent pain programs. Multidisciplinary courses radiate here. Discover to stage goals by function, sleep, and engagement before pain strength. Change interest toward values‑based activity. Manual inputs continue to be, yet you stop chasing full relief and start measuring significant gains.
What to try to find when you assess a course
Marketing can be loud. Strip it back to basics. Is the training course practical, or is it selling certainty? Do trainers demonstrate scientific reasoning on untidy instances, not only book instances? Are dosage and decision policies specific? Are technique specifications showed along with weaning methods? Will certainly you exercise conversations that minimize threat without rejecting pain?
The most beneficial pain monitoring training programs that I have actually seen share 3 attributes. Initially, they start with assessment shapes your strategy, not an automatic technique. Second, they respect time. You leave with a 30 to 45‑minute evaluation theme you can use tomorrow, scalable to 20‑minute follow‑ups. Third, they gather information. You learn to track end results that matter to individuals, like the variety of uninterrupted sleep hours or the capacity to lift a grandchild, not just levels and millimeters.
Practical guidebook methods that hold up
In daily method, a handful of hands-on strategies consistently unlock to motion when used with treatment. Cervical and thoracic mobilizations to boost neck turning and minimize frustration intensity. Lumbar side glides and basic posterior‑anterior mobilizations to feed motion into a guarded back. Hip distraction with movement for rigid hips that limit stride. Soft tissue work around the proximal hamstring to calm a re‑flaring runner. Peripheral nerve methods like ulnar nerve sliders for median joint discomfort coupled with grip and shoulder strength.
Each strategy requires a why and a what next off. If a thoracic mobilization boosts a shoulder's elevation by five degrees and minimizes pain on reach, quickly catch it with wall surface slides and light lugs. If a hip distraction enables pain‑free sit‑to‑stand, adhere to with pace squats to build tolerance.
Using modalities so they offer the plan
It helps to pre‑decide exactly how you will utilize a method instead of improvisating in fatigue. As an example, TENS comes to be a short‑term analgesic for jobs that matter: food preparation, initial stroll of the early morning, or post‑therapy home technique. Heat comes to be a nighttime training in pain management techniques pre‑sleep routine for people with high tone. Shockwave shows up just after at least eight to twelve weeks of dynamic loading and adherence in stubborn tendinopathy, with clear exit criteria. Ultrasound is rarely used besides a protocol‑driven sign, and even after that, notified approval includes its limited effect size.
This framework maintains methods in a sustaining duty and safeguards clinic time for mentoring and movement.
How nurses, physios, and teams align
Many centers run mixed groups. Discomfort administration training courses for registered nurses frequently stress secure analgesic administration, surveillance, and patient education on medications. Pain management training for nurses that overlaps with physical rehabilitation around positioning, very early mobilization, and pacing brings real dividends. Joint case assesses decrease blended messages. When both registered nurse and physio utilize the same flare‑up plan and task ladders, clients stop bouncing in between suggestions and begin progressing.
Where credentialed nurses finish a pain administration certificate or pain monitoring accreditation training course that includes non‑pharmacological techniques, physios can sync by straightening language and enhancing movement‑based approaches. The factor is uniformity. People gravitate to in agreement messages.
Managing flare‑ups without thwarting progress
Flare ups are not failure. Training courses that teach proactive flare‑up preparation save hours of facility time. I show clients a three‑day policy. The first day, minimize tons by roughly one 3rd, keep simple activity every hour, add warmth or TENS if it helps. Day two, repeat if needed and test a couple of motions that previously felt secure. Day three, attempt go back to baseline filling minus one variable, like less sets or reduced variety, and track feedback. If pain trends down, resume the program. If it stalls or intensifies, call me sooner.
This method develops self‑efficacy and reduces dependancy on last‑minute appointments. It likewise requires us to compose programs with handles you can turn: pace, array, exterior tons, frequency, complexity.
Assessment anchors that assist change
Pain strength alone floats with sleep, tension, and weather condition. Much more secure anchors help. I request for one meaningful feature, one participation objective, and one sleep statistics. For feature, it could be staircase tolerance or unloaded squat deepness. Engagement might be an once a week football game or a complete job change without break. Sleep could be total hours or the variety of awakenings. These produce a dashboard that both people can influence. Hand-operated treatment may bump staircase resistance today. A pacing plan might secure the work change this week. Breathwork and warmth may add an hour of sleep by the weekend. That noticeable progress builds trust fund also when pain lingers.
Building your path: from brief course to certification
If you are early in your job, start with brief courses hurting administration that hone a slim set of abilities and examine them in facility the following week. Two instances that normally pay off promptly are hand-operated therapy dosing and interaction for pain education. As cases expand a lot more intricate, include modules on rated electric motor imagery, CBT‑informed activity pacing, and neuropathic pain.
For medical professionals aiming to formalize know-how, a discomfort monitoring certificate training course can be worth the investment if it includes monitored instances, gauged end results, and a capstone that integrates hands-on treatment, modalities, and training. Beware of programs that promise quick pain cures or count on a solitary modality as the centerpiece. Breadth with deepness wins.
If your solution runs acute pathways, add emergency situation discomfort administration training that clarifies warning screens, secure placements of ease, and the line in between movement analgesia and medical acceleration. In some regions, program content will certainly reference units like PUAEME008 offer discomfort management to standardize emergency situation feedback actions. Also when your scope continues to be non‑pharmacological, the common structure helps you function cleanly with ED groups and paramedics.
Two compact tools you can make use of tomorrow
The min facility is genuine. You frequently have just a couple of mins to make a dent. Below are two tools that compress well inside active appointments.
- The 3‑by‑3 description. Three sentences on what pain indicates for this case, 3 sentences on what we will certainly do today, and 3 sentences on what you will do at home. It maintains you from over‑explaining and keeps the individual from leaving confused. The home window and wedge approach. Discover a strategy that opens a tiny home window of minimized pain or far better movement, then wedge it open with a matched job. For an unpleasant shoulder, the home window could be a thoracic mobilization, and the wedge may be wall slides with regulated breath. For a hot back, the window might be side glides, and the wedge could be short collections of hip‑hinge practice.
Used regularly, these little patterns develop momentum and conserve your time.
Measuring worth past the session
A training course that transforms technique will transform your schedule. You will spend much less time chasing pain scores and more time organizing developments. Reflect on in brief yet meaningful methods. Fifteen seconds to reconsider a practical task can be a lot more informative than five mins of array dimensions. Ask the sleep inquiry near the beginning of each visit. If rest has actually gone down, change load or add a recovery intervention. When a modality makes a look, attach a leave plan. That accountability protects against drift into passive treatment as the default.
Final thoughts from the treatment room
After fifteen years in clinics that range from weekend break sports to healthcare facility wards, the pattern holds. Pain eases when the plan respects biology, ideas, and actions at the same time. Manual therapy offers you touch and timing. Techniques give you alternatives when the floor is warm. Education provides your individual the map. Programs that build these together deserve your time and money.
A good pain administration training course does not make you choose between hands and head. It reminds you that both issue, and it shows you just how to utilize them in the right order. Whether you go after a discomfort administration qualification or keep piling brief courses, go for training that elevates choices, clarifies communication, and delivers alter your people can feel in the initial couple of brows through. That is the type of worth that maintains individuals returning, except easy care, but also for partnership.